- This information was developed by GMR Web Team.
- This information is intended only to provide general guidance. It does not provide definitive medical advice.
- It is important that you consult your doctor about your specific condition.
Psoriasis
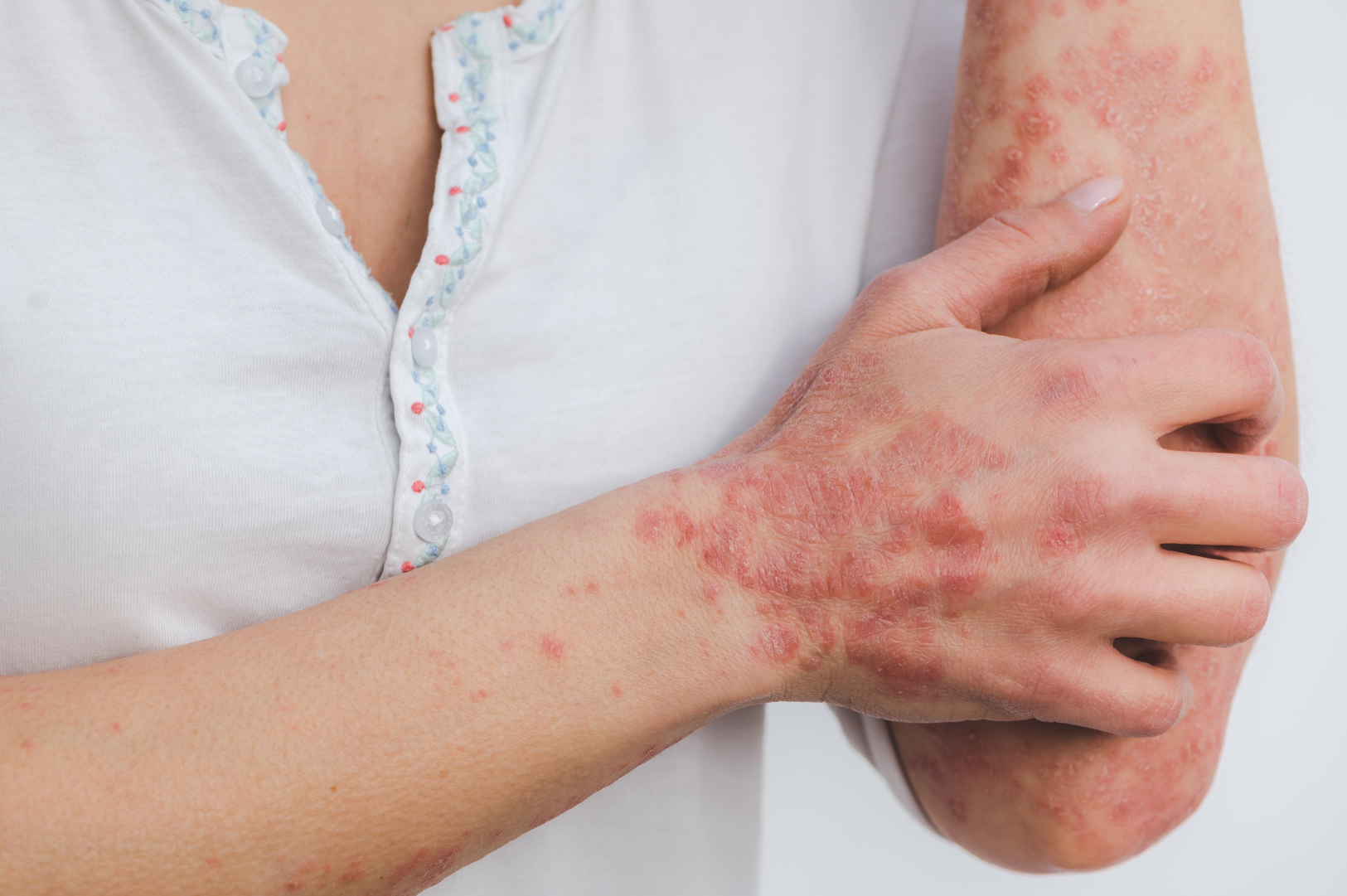
Psoriasis is an autoimmune (a disease that occurs when your body’s natural defense system mistakenly attacks healthy cells and tissues) skin condition that causes dry, scaly skin with severe redness and itchiness. A psoriasis rash can occur anywhere in the body but is commonly seen on your elbows, knees, face, scalp, lower back, palms, and feet. Most often, psoriasis rash covers a small area of your skin; however, in severe cases, the rashes can connect and cover a large area of your body. While there is no cure for psoriasis, dermatologists (doctors specializing in diagnosing and treating conditions and diseases affecting the skin, hair, and nails) can help manage the symptoms. Your doctor may prescribe medicated creams or ointments for psoriasis.
Let's delve into the types, causes, triggering factors, symptoms, treatment, and complications of psoriasis to better understand the condition.
What is Psoriasis?
Psoriasis is a chronic (long-lasting) autoimmune disease affecting the skin due to an overactive immune system. An abnormal and rapid multiplication of the skin cells results in an inflammatory reaction, causing thick, scaly patches called plaques. Plaques often appear on your face, scalp, elbows, knees, and other body parts.
What Are the Types of Psoriasis?
There are several types of psoriasis, namely:
Plaque Psoriasis
- This is the most common type of psoriasis that forms thick, itchy scales called plaques.
Inverse Psoriasis
- This psoriasis develops in your skin folds that cause thin, scaly plaques.
Guttate Psoriasis
- This type of psoriasis often occurs after an episode of sore throat.
- The rash resembles a small, red, drop-shaped scaly spot commonly affecting children and young adults.
Pustular Psoriasis
- This type of psoriasis results in small, pus-filled bumps over the plaque areas.
Erythrodermic Psoriasis
- This is considered the most severe form of psoriasis affecting larger areas of your skin.
- It is characterized by widespread skin discoloration and shedding.
Sebopsoriasis
- This type typically appears as tiny bumps and plaques on your face and scalp.
Nail Psoriasis
- This type of psoriasis affects your nails, causing discoloration, pitting, and disfigurement of your fingers and toenails.
What Causes Psoriasis?
Though the cause of psoriasis remains a mystery, decades of scientific research reveals the role of the following factors:
Immune System
- Psoriasis is an autoimmune skin disease, which means an overactive immune system causes inflammation in your skin. Instead of destroying foreign invaders like bacteria, your immune system mistakes healthy cells for foreign invaders and destroys them.
- This leads to an inflammatory reaction in the body, which appears as red, thick, scaly rashes, bumps, or plaques on the skin surface.
- The skin cell destruction and growth cycle are disrupted, and the time taken for new cell growth is 3 to 4 days instead of the usual 30 days.
- The speed with which new cells replace old cells creates scales and frequent shedding of the skin on top of plaques.
Genetics
- You may inherit the genes that make you more susceptible to developing psoriasis.
- A parent, sibling, or an immediate family member can increase your likelihood.
Are There Any Risk Factors for Psoriasis?
Several risk factors can make you more prone to develop psoriasis. These include:
- Inflammatory bowel disease
- Infections like bronchitis, strep throat, and tonsillitis
- Cardiovascular disease
- Diabetes
- Smoking
- Obesity
- Hypertension
- Hormonal changes
What Can Trigger Psoriasis?
External triggers may start an outbreak of psoriasis or cause a flare-up. Common triggers include:
- Stress and anxiety
- Excess alcohol consumption
- Injury like a cut, scratches, burns, or bites
- Medications such as beta-blockers, lithium, antimalarials, tetracycline, and NSAIDs (non-steroidal anti-inflammatory drugs)
- Infection caused by streptococcal bacteria
- Environmental Factors like sudden changes in the body temperature
What Are the Symptoms of Psoriasis?
The symptoms of psoriasis may depend on your psoriasis and may differ from person to person. The most common symptoms include:
- Areas of raised, inflamed skin patches that appear red on light skin tone and brownish-purple on dark skin tone
- Red patches consist of whitish-silver scales over them, while the brown patches have gray scales
- The affected skin may be dry, cracked, or inflamed
- The affected skin may bleed easily
- Soreness and tenderness around the patches
- Itching and burning sensation in the skin around the patches
- Thick, pitted nails
- Painful, tender, inflamed, and swollen joints (psoriasis arthritis)
- Skin ulceration occurs if you accidentally scratch and break open your skin
How is Psoriasis Diagnosed?
Dermatologists can diagnose psoriasis with the following:
Medical History
- Your doctor will record your symptoms and medical history to evaluate your genetic background and lifestyle habits (smoking, alcohol, etc.)
Physical Examination
- Your doctor will clinically evaluate your skin rash to evaluate its appearance and severity.
Skin Biopsy Test
- If the symptoms are unclear, your doctor will order a skin biopsy test to confirm the suspected diagnosis.
- A small skin sample around the plaque or rash is extracted and sent to a lab for analysis.
- This can confirm psoriasis or rule out other possible infections and disorders.
How is Psoriasis Treated?
There is no definite cure for psoriasis, but several treatment options can help manage the symptoms. The treatment aims to reduce inflammation, slow the growth of skin cells, and help eliminate plaques.
Treatment options include:
Topical Treatments
- These are available as creams, lotions, and ointments for mild to moderate psoriasis. These include:
- Retinoids
- Corticosteroids
- Anthralin
- Vitamin D
- Salicylic acid
- Moisturizers
Systemic Medications
- These medications are used for moderate to severe psoriasis, either orally or through injectables. These include:
- Retinoids
- Methotrexate
- Cyclosporine
- Biologics
Light Therapy
- This method uses UV or natural light to kill the overactive white blood cells that attack healthy cells and cause rapid cell growth.
- It is helpful to treat moderate to severe forms of psoriasis.
What Are the Complications of Psoriasis?
Following are some of the complications of psoriasis that you may encounter if the condition is not managed appropriately.
- Psoriatic arthritis with painful, stiff, swollen joints.
- Vision troubles include symptoms such as red eyes, blurry vision, teary eyes, asymmetrical pupils, and increased sensitivity to light.
- Hair loss due to scalp psoriasis
- Increased risk of cancer and heart failure
- Anxiety and depression
Bottom Line
Psoriasis is an itchy skin condition due to an overactive immune response. Though it is not contagious, the skin changes can bother and require medical care. Psoriasis does not have a definite cure, but psoriasis treatment can improve symptoms and overall quality of life. Your doctor may prescribe topical creams, lotions, or systemic medications (oral and injectables). Severe forms of psoriasis may be relieved by special therapies like light therapy.
Consult your dermatologist immediately if you notice any abnormal bump, rash, or scaly plaque.
